Traumatic Brain Injury (TBI): Rehabilitation, Therapy, and Recovery
214,110
TBI-related hospitalizations in the U.S. in 2020
69,473
TBI-related deaths in the U.S. in 2021
10–20%
May experience persistent symptoms after mild TBI
OT • PT • SLP
TBI rehabilitation disciplines
Executive Function
Indicator of long-term functional limitation after TBI

Key Takeaways
- Approximately 2.87 million TBI-related emergency department visits occur in the United States each year (Haarbauer-Krupa et al., 2021)
- An estimated 43% of those hospitalized with TBI experience long-term disability (Haarberg-Krupa et al., 2021)
- Falls are the leading cause of TBI across all age groups (CDC, 2024)
- TBI affects cognition (thinking and memory), communication, motor function, and emotional regulation
- Multidisciplinary rehabilitation — including OT, PT, and SLP — improves functional outcomes across all TBI severities
- Long-term disability is common after severe TBI, underscoring the need for ongoing rehabilitation support (Mostert et al., 2022)
Important
The information on this page is educational only and is not a substitute for a clinical evaluation, diagnosis, or individualized therapy recommendations. If you or someone you care for has experienced a head injury, speak with a qualified healthcare professional as soon as possible — early evaluation and treatment produce the best outcomes.
Table of Contents
- What Is Traumatic Brain Injury?
- How Is TBI Classified?
- Who Is at Risk?
- Who Provides Therapy for People with TBI?
- Occupational Therapy in TBI Rehabilitation
- Physical Therapy and Motor Recovery
- Speech-Language Pathology in TBI
- Cognitive Rehabilitation
- Emotional and Behavioral Changes
- Community Reintegration and Return to Work
- What Families Can Do
- A Note for Clinicians
- References
1. What Is Traumatic Brain Injury?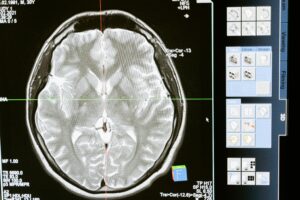
Traumatic brain injury (TBI) occurs when a sudden external force — such as a blow, jolt, or penetrating injury — disrupts normal brain function. TBI is not a single condition but a broad category of injuries that vary widely in cause, severity, and outcome. Effects can range from brief changes in consciousness to permanent cognitive and physical impairment (CDC, 2024).
TBI is a leading cause of death and long-term disability in the United States. An estimated 2.87 million TBI-related emergency department visits, hospitalizations, and deaths are reported annually, and approximately 43% of those hospitalized will experience long-term disability (Haarbauer-Krupa et al., 2021). These figures likely underestimate the true burden, as many mild TBIs — particularly concussions — go unreported or are managed outside of hospital settings (Waltzman et al., 2025).
The effects of TBI reach far beyond the brain. Depending on the location and severity of injury, TBI can affect movement, communication, thinking and memory (cognitive function), emotional regulation, and the ability to participate in work, school, and daily life. Related pages on this site address many of these areas — including fall prevention, adaptive feeding, and stroke recovery, which shares many rehabilitation principles with TBI.
2. How Is TBI Classified?
TBI is typically classified by severity using the Glasgow Coma Scale (GCS), a standardized tool that measures eye opening, verbal response, and motor response following injury. Scores range from 3 to 15, with lower scores reflecting more severe injury.
- Mild TBI (GCS 13–15): Also called concussion. Involves brief or no loss of consciousness, short-term confusion, or a gap in memory. Accounts for 75–80% of all TBIs (Haarbauer-Krupa et al., 2021).
- Moderate TBI (GCS 9–12): Involves loss of consciousness lasting minutes to hours and more significant cognitive and physical effects.
- Severe TBI (GCS 3–8): Involves prolonged unconsciousness and often results in lasting cognitive, physical, and behavioral impairments. Mortality rates range from 18–75%, and unfavorable outcomes are reported in 29–100% of survivors (Mostert et al., 2022).
TBI may also be classified as primary (damage occurring at the moment of impact) or secondary (additional brain damage developing in the hours and days after the initial injury due to swelling, reduced oxygen, or increased pressure in the skull). Secondary injury is a key target of early medical and rehabilitation intervention.
A Note on “Mild” TBI
The term “mild” refers to the initial classification based on loss of consciousness — not the person’s long-term experience. Some individuals with mild TBI experience persistent symptoms — headaches, difficulty concentrating, sleep disturbances, and emotional changes — that significantly affect daily functioning for weeks, months, or longer. These persistent symptoms are real and warrant clinical attention (Waltzman et al., 2025).
3. Who Is at Risk?
TBI affects people across all ages, but certain groups face higher risk (Haarbauer-Krupa et al., 2021; CDC, 2024): 
- Young children (ages 0–4) and older adolescents (ages 15–19) have the highest rates of TBI-related emergency department visits
- Adults aged 75 and older have the highest rates of TBI-related hospitalizations and death, largely due to falls
- Males experience TBI at approximately 1.6 times the rate of females across all age groups
- Falls are the leading overall cause of TBI — motor vehicle crashes and being struck by or against an object are also major contributors (CDC, 2024)
- Military veterans represent a significant population affected by TBI, often due to blast exposure
For Patients & Families
- Falls are the leading cause of TBI — fall prevention strategies are among the most important protective measures for older adults and young children
- Wearing helmets during cycling, skating, skiing, and contact sports significantly reduces TBI risk and severity
- Any head injury that involves loss of consciousness, confusion, memory gaps, or worsening headache should be evaluated by a medical professional promptly
- Even a “mild” concussion in a child or older adult warrants medical evaluation — these age groups are at higher risk for complications
4. Who Provides Therapy for People with TBI?
TBI rehabilitation requires a multidisciplinary team because the injury can affect nearly every system of the body. Effective care is coordinated across disciplines and adjusted as the person’s needs change through the stages of recovery (Shen et al., 2025; Mostert et al., 2022).
- Occupational therapy (OT): Cognitive rehabilitation, daily living skills, return to work, home safety, driver rehabilitation, and community participation
- Physical therapy (PT): Mobility, balance, strength, coordination, and motor recovery
- Speech-language pathology (SLP): Communication, swallowing, and cognitive-communication skills
- Neuropsychology: Comprehensive assessment and treatment of cognitive and emotional changes
- Neurology/physiatry (rehabilitation medicine): Medical management, medication, and care coordination across the team
- Social work: Community resources, caregiver support, return to school or work planning, and insurance navigation
Evidence consistently supports early referral to multidisciplinary rehabilitation, as coordinated team care is associated with better functional outcomes across mild, moderate, and severe TBI (Shen et al., 2025; Mostert et al., 2022).
For Clinicians
- Multidisciplinary referral should be initiated early — coordinated team care produces better outcomes than single-discipline management across all TBI severities (Shen et al., 2025).
- For mild TBI: do not assume symptoms will resolve without support. Persistent post-concussion symptoms warrant OT and SLP evaluation even when neuroimaging is normal (Waltzman et al., 2025).
- Reassess rehabilitation needs at every major transition — hospital discharge, return to school or work, and any significant functional change are all triggers for re-referral.
5. Occupational Therapy in TBI Rehabilitation
Occupational therapy addresses the full range of daily activities that TBI can disrupt — from basic self-care such as dressing and bathing to complex tasks like managing finances, driving, and returning to work. OT focuses on helping individuals regain functional independence and meaningful participation in life roles (Mullins et al., 2025; Shen et al., 2025).
Key areas of OT intervention in TBI include:
- Activities of daily living (ADLs): Relearning or adapting routines for dressing, grooming, meal preparation, and medication management
- Cognitive strategies: Teaching compensatory techniques — strategies that work around deficits rather than eliminating them — for memory, attention, and organization
- Home safety and environmental modification: Assessing and modifying the home to reduce fall risk and support independence
- Driver rehabilitation: Evaluating readiness and providing training for safe return to driving after TBI
- Community reintegration: Supporting return to school, work, and social participation
A 2025 systematic review found moderate-level evidence that multidisciplinary and holistic OT approaches support successful return to work and community reintegration for individuals with TBI (Mullins et al., 2025). A comprehensive review of TBI rehabilitation approaches confirmed that occupational therapy, combined with cognitive and psychosocial interventions, improves functional independence and quality of life in moderate-to-severe TBI (Shen et al., 2025).
For Patients & Families
- Difficulty with daily tasks after a brain injury is expected — it is not a sign of permanent limitation
- OT can help develop strategies to compensate for cognitive changes, even when full recovery is not possible
- Goals are individualized — what matters most is what helps the person participate in their own life, work, and relationships
- It is never too late to seek OT — people can continue to make meaningful gains long after the initial injury
For Clinicians
- A 2025 systematic review confirmed moderate-level evidence for multidisciplinary and holistic OT approaches in improving return-to-work outcomes after TBI — vocational goals should be incorporated into OT planning from early in the rehabilitation process (Mullins et al., 2025).
- Driver rehabilitation after TBI requires specialized OT assessment — standard medical clearance is insufficient. Refer to a certified driver rehabilitation specialist (CDRS) when driving is a goal.
- Home safety assessment before discharge is a high-yield intervention — fall risk is significantly elevated in TBI survivors, particularly those with balance, attention, or processing speed deficits.
6. Physical Therapy and Motor Recovery
Motor impairments — including weakness (hemiparesis), balance problems, coordination difficulties, and gait disturbances — are common following moderate and severe TBI. Physical therapy targets these deficits with the goal of improving mobility, reducing fall risk, and maximizing functional independence.
Exercise and movement-based interventions are supported by evidence across TBI severities. Task-specific training — practicing actual functional movements like walking, reaching, and climbing stairs — and neuroplasticity-based approaches are central to PT for TBI. Balance training and fall prevention are especially important for older adults and those with persistent postural instability (Shen et al., 2025).
For Patients & Families
- Physical recovery from TBI can be slow — early progress may be followed by plateaus, then further gains. Neuroplasticity continues well beyond the acute phase
- Balance and gait problems, even subtle ones, increase fall risk and should be formally evaluated by a physical therapist (CDC, 2024)
- Staying physically active supports both motor and cognitive recovery — ask your PT what exercises are safe and beneficial for your specific situation
- A physical therapist can develop a safe home exercise program matched to current abilities — do not wait until symptoms are severe to request a referral
For Clinicians
- Task-specific, high-repetition training is more effective than passive modalities for motor recovery in TBI — therapy sessions should be active and functionally meaningful (Shen et al., 2025).
- Dual-task assessment — evaluating balance or gait while performing a concurrent cognitive task — is essential in TBI given the frequency of combined motor and cognitive deficits that interact to increase fall risk.
- Fall risk assessment should be performed and documented at every care transition — falls in TBI survivors are common, underreported, and frequently preventable with appropriate PT intervention.
7. Speech-Language Pathology in TBI
TBI frequently affects communication and swallowing. Speech-language pathologists (SLPs) address a range of TBI-related challenges including (Shen et al., 2025):
- Dysarthria: Slurred or unclear speech caused by weakness or incoordination of the speech musculature
- Aphasia: Difficulty finding or understanding words — less common in TBI than in stroke but can occur with focal injury
- Cognitive-communication disorders: Difficulty organizing thoughts, following conversations, staying on topic, or understanding implied meaning — even when basic speech appears intact. This is the most common communication consequence of TBI.
- Dysphagia (swallowing difficulty): Can occur after severe TBI and carries risks of aspiration, aspiration pneumonia, malnutrition, and dehydration — see our adaptive feeding page for more on dysphagia management
Cognitive-communication deficits are among the most persistent and functionally limiting consequences of TBI, affecting social relationships, employment, and daily functioning. Evidence supports SLP intervention across the TBI severity spectrum, with particular emphasis on functional communication in real-life contexts (Shen et al., 2025).
For Patients & Families
- If a person with TBI struggles in conversations, becomes confused or disorganized, or has difficulty following complex discussions, this may reflect cognitive-communication impairment — not a lack of effort or intelligence
- Speech therapy can be highly effective even months or years after injury — neuroplasticity supports continued communication gains well beyond the acute phase
- Swallowing concerns — coughing during meals, unexplained weight loss, a wet voice after eating, or changes in eating habits — warrant prompt SLP evaluation
- Augmentative and alternative communication (AAC) devices — from simple boards to high-tech speech-generating devices — can restore meaningful communication for those with severe dysarthria
For Clinicians
- Cognitive-communication disorders are the most common and functionally significant communication consequence of TBI — they are frequently missed when assessment focuses only on speech intelligibility and basic language tasks.
- Formal discourse analysis and functional communication assessment in natural contexts is more sensitive to TBI-related communication deficits than standardized aphasia batteries.
- Dysphagia after TBI is often underdetected — particularly in the acute phase when medical status is fluctuating. Routine swallowing screening before oral intake is standard of care following severe TBI.
8. Cognitive Rehabilitation
Cognitive rehabilitation — treatment designed to address impairments in attention, memory, processing speed, and executive function (the ability to plan, organize, and solve problems) — is a central component of TBI care across all severity levels.
Approaches include both restorative strategies (structured exercises intended to improve the underlying cognitive ability) and compensatory strategies (tools and techniques that help a person function effectively despite cognitive limitations, such as using calendars, checklists, alarms, and structured routines). A scoping review of studies from 2015–2021 found clinically significant effects of cognitive rehabilitation in 93% of studies reviewed, with 41% reporting improvement on the primary outcome measure (Julien et al., 2023).
Addressing cognitive impairment is a priority across OT, SLP, and neuropsychology — and the approach should be coordinated across disciplines to ensure consistent strategy use in all settings, not just therapy sessions.
For Patients & Families
- Cognitive changes after TBI — memory difficulties, slower thinking, trouble concentrating — are neurological, not a sign of laziness or lack of motivation
- Compensatory strategies — like using a phone calendar, written checklists, and consistent daily routines — can dramatically improve daily functioning even when the underlying cognitive deficit does not fully resolve
- A 2023 scoping review found clinically significant effects of cognitive rehabilitation in 93% of studies — this is a well-supported area of TBI treatment worth pursuing (Julien et al., 2023)
- Fatigue significantly worsens cognitive performance in TBI — managing energy levels throughout the day is as important as the cognitive strategies themselves
For Clinicians
- Standardized cognitive screening tools such as the MoCA or CLQT are useful for initial identification of deficits, but functional assessment during real-world tasks is essential — structured testing frequently overestimates real-world cognitive capacity in TBI (Julien et al., 2023).
- Cognitive performance can fluctuate significantly based on fatigue, pain, medication, and environmental demands — assess at multiple time points and document variability.
- Attend to the gap between structured testing performance and everyday functioning — this gap often reveals the most clinically relevant information and guides the selection of compensatory versus restorative approaches.
- Cognitive rehabilitation outcomes are significantly improved when strategies are practiced consistently across all settings — coordination between OT, SLP, neuropsychology, and family members is essential.
9. Emotional and Behavioral Changes
Emotional and behavioral changes are among the most challenging and often least anticipated consequences of TBI. These changes are neurological in origin — meaning they result directly from brain injury — and are not simply a reaction to stress or an inability to cope.
Common changes include depression, anxiety, irritability, impulsivity (acting without thinking), emotional lability (rapid or exaggerated emotional shifts), and apathy (reduced motivation or initiation). Moderate and severe TBI can cause significant personality changes including severe irritability, affective instability, and impulsivity, while even mild TBI is associated with increased risk of depression and anxiety (Howlett & Stein, 2022).
Psychological support, behavioral strategies, and in some cases medication management are all part of comprehensive TBI care. Untreated emotional and behavioral changes are among the strongest predictors of poor long-term outcomes after TBI (Howlett & Stein, 2022).
For Patients & Families
- Personality or emotional changes after a brain injury are a result of the injury itself — not a character flaw, a choice, or a failure of willpower
- Depression and anxiety after TBI are neurobiological conditions that respond to treatment — report mood changes to the care team and request a psychology or psychiatry referral (Howlett & Stein, 2022)
- Families often carry a significant caregiving burden — support for caregivers is a legitimate and important part of TBI care, not a luxury
- If a family member with TBI is showing signs of significant depression, increasing irritability, social withdrawal, or loss of motivation, report this to the rehabilitation team promptly
For Clinicians
- Emotional and behavioral changes after TBI are neurological — they require the same clinical attention and systematic assessment as motor or cognitive deficits. Screening for depression and anxiety should be routine at every episode of care (Howlett & Stein, 2022).
- Anosognosia (reduced self-awareness of deficits) is common after TBI — the person may not recognize their own mood or behavioral changes. Collateral history from family members is essential.
- Impulsivity and reduced inhibition can create safety risks — driving, financial decisions, and medication management should all be evaluated in the context of behavioral control deficits.
- Caregiver burden is a significant predictor of both patient and family outcomes — assess it proactively and refer to caregiver support resources as a standard part of the care plan.
10. Community Reintegration and Return to Work
Returning to meaningful participation in community life — including work, school, relationships, and leisure — is a primary long-term goal of TBI rehabilitation. Many individuals with TBI face persistent challenges in these areas long after the acute phase of recovery.
Return to work following TBI is influenced by injury severity, cognitive and emotional functioning, workplace demands, and availability of support. A 2025 systematic review found that multidisciplinary and holistic rehabilitation approaches — including vocational rehabilitation (job-focused therapy), cognitive and mental health interventions, and client-centered care — provide moderate-level evidence for improved return-to-work outcomes (Mullins et al., 2025).
Social participation and community engagement remain important beyond employment. Isolation is a common and underaddressed consequence of TBI. Supported participation in community activities, peer support programs, and structured social opportunities can meaningfully improve quality of life for individuals at all stages of recovery (Shen et al., 2025).
For Patients & Families
- Return to work or school after TBI is a realistic goal for many people — but it often requires a gradual, supported process rather than a sudden full return
- Workplace or school accommodations — modified hours, reduced cognitive load, written instructions, quiet workspaces — can make the difference between successful return and repeated failure
- Vocational rehabilitation services are available in every state — ask your OT or social worker for a referral
- Social isolation is a serious and common consequence of TBI — maintaining relationships, community involvement, and peer connections is important for long-term quality of life (Shen et al., 2025)
For Clinicians
- Vocational goals should be incorporated into rehabilitation planning from early in the recovery process — not added as an afterthought at discharge (Mullins et al., 2025).
- Driving is a critical community participation goal for many adults with TBI — it requires specialized OT driver rehabilitation evaluation, not simply medical clearance from a physician.
- Social isolation is significantly underaddressed in TBI rehabilitation — assess community participation and social engagement proactively.
11. What Families Can Do
Family involvement is consistently identified as an important factor in TBI recovery outcomes. Caregivers and family members play a central role in supporting skill generalization — helping the person practice and apply strategies learned in therapy in everyday life (Shen et al., 2025; Mullins et al., 2025).
- Learn about your family member’s specific deficits: Understanding the cognitive, emotional, and behavioral changes caused by TBI helps you respond effectively rather than reactively
- Establish consistent routines and environments: Predictability reduces cognitive load and supports memory and organization for people with TBI
- Encourage independence: Allow the person to attempt tasks independently before offering assistance — maintaining active engagement supports neuroplastic recovery and preserved dignity
- Attend therapy sessions when possible: Observing therapy allows you to learn strategies and reinforce them at home — where generalization matters most
- Communicate proactively with the rehabilitation team: Share what you are observing at home — changes in mood, behavior, safety, or function that the individual may not be aware of themselves
- Seek support for yourself: Caregiver burden after TBI is real and significant. Brain Injury Alliance and BIAA offer caregiver resources nationally.
When to Request a Therapy Referral
- Following any head injury that involves loss of consciousness, confusion, or a gap in memory — even briefly
- When symptoms persist beyond a few weeks after a concussion or mild TBI
- When daily tasks such as cooking, managing finances, or returning to work feel difficult or overwhelming
- When emotional or behavioral changes are affecting relationships or daily functioning
- At any transition point — discharge from hospital, return to school or work, or major life change
- When a family member or caregiver notices changes in thinking, behavior, or safety that the individual may not recognize themselves
- When swallowing concerns are present — coughing during meals, unexplained weight loss, or changes in eating habits
- Any concern is a valid reason to seek evaluation — early referral consistently supports better long-term outcomes
12. A Note for Clinicians
TBI presentation is highly variable and does not always correlate neatly with initial injury severity. Individuals with mild TBI may present with functionally significant deficits that are invisible on standard neuroimaging. Conversely, some individuals with moderate or severe TBI achieve substantial recovery with intensive rehabilitation (Waltzman et al., 2025; Mostert et al., 2022).
Functional observation across real-world tasks remains essential. Standardized assessment provides useful baseline data, but performance in clinical settings frequently underestimates the demands — and overestimates functional capacity — relative to daily life. Fatigue, pain, and reduced self-awareness (anosognosia — difficulty recognizing one’s own deficits) are common and interact with both assessment accuracy and rehabilitation participation.
Caregiver education and family engagement are not supplemental to TBI rehabilitation — they are a core component. Research consistently links caregiver involvement to improved outcomes, particularly in the areas of skill generalization, emotional regulation, and community reintegration (Mullins et al., 2025; Shen et al., 2025).
The evidence base for TBI rehabilitation has strengthened considerably in recent years. A 2025 comprehensive review confirmed that multidisciplinary rehabilitation — combining OT, PT, SLP, neuropsychology, and psychosocial support — produces better outcomes than any single-discipline approach. The quality and intensity of rehabilitation, not only the severity of injury, significantly shapes long-term functional outcomes (Shen et al., 2025).
Related Pages on TherapyTopics
- Stroke Recovery and Rehabilitation — OT, PT, and SLP after stroke — neuroplasticity, ADL retraining, and caregiver guidance
- Fall Prevention — Balance assessment, home hazard reduction, and evidence-based exercise programs for older adults
- Adaptive Feeding — Dysphagia management, adaptive equipment, and evidence-based feeding intervention
- Dementia & Alzheimer’s Disease — Cognitive rehabilitation, ADL support, and caregiver training
- Sensory Processing & Integration — Sensory differences affecting daily function and participation
13. References
- Centers for Disease Control and Prevention. (2024). Traumatic brain injury & concussion: Data and statistics. National Center for Injury Prevention and Control. https://www.cdc.gov/traumatic-brain-injury/data-research/index.html
- Haarbauer-Krupa, J., Pugh, M. J., Prager, E. M., Harmon, N., Wolfe, J., & Yaffe, K. (2021). Epidemiology of chronic effects of traumatic brain injury. Journal of Neurotrauma, 38(23), 3235–3247. https://doi.org/10.1089/neu.2021.0062
- Howlett, J. R., & Stein, M. B. (2022). Mental health consequences of traumatic brain injury. Biological Psychiatry, 91(5), 413–420. https://doi.org/10.1016/j.biopsych.2021.09.024
- Julien, A., Danet, L., Loisel, M., Brauge, D., Pariente, J., Péran, P., & Planton, M. (2023). Update on the efficacy of cognitive rehabilitation after moderate to severe traumatic brain injury: A scoping review. Archives of Physical Medicine and Rehabilitation, 104(2), 315–330. https://doi.org/10.1016/j.apmr.2022.07.007
- Mostert, C. Q. B., Singh, R. D., Gerritsen, M., Kompanje, E. J. O., Ribbers, G. M., Peul, W. C., & van Dijck, J. T. J. M. (2022). Long-term outcome after severe traumatic brain injury: A systematic literature review. Acta Neurochirurgica, 164(3), 599–613. https://doi.org/10.1007/s00701-021-05086-6
- Mullins, A., Scalise, O., Carpio-Paez, B., DeShaw, V., Jennings, K., Kitchens, R., Hilton, C., & Mani, K. (2025). Occupational therapy interventions in facilitating return to work in patients with traumatic brain injury: A systematic review. Work, 81(2), 2458–2476. https://doi.org/10.1177/10519815251317411
- Shen, Y., Jiang, L., Lai, J., Hu, J., Liang, F., Zhang, X., & Ma, F. (2025). A comprehensive review of rehabilitation approaches for traumatic brain injury: Efficacy and outcomes. Frontiers in Neurology, 16, 1608645. https://doi.org/10.3389/fneur.2025.1608645
- Waltzman, D., Black, L. I., Daugherty, J., Peterson, A. B., & Zablotsky, B. (2025). Prevalence of traumatic brain injury among adults and children. Annals of Epidemiology, 103, 40–47. https://doi.org/10.1016/j.annepidem.2025.02.005
© TherapyTopics.com — All information is for educational purposes only and does not constitute medical or therapeutic advice. Consult a licensed therapist or physician for evaluation and treatment.

